Nursing: Empathy in Person Centered Care
Question:
Discuss about the Nursing for Empathy in Person Centered Care.
Answer:
The nurse completes an assessment of Mr Barber’s condition on arrival. Explain the following in relation to the assessment process.
Discuss the type of infection control policy would be implemented for Mr Barber?
The infection control policy for emphysema would involve manipulating the situation to lessen and mitiage the pains of the ailment. This includes organising for practical help, creating routines that would ensure that treatment models are followed. Proper explanations have to be made and understood regarding the patient’s disease, to enable the doctor match the medical conditions with the understanding which the doctor has understood about the disease.
List the PPE precautions that the nurse would use during assessment
PPE referes to an equipmemt used to create a barrier between the various harmful equipment and the patient’s body, to prevent any direct contact and transfer of germs. The first PPE precaution involves loweriung the temperature setting on the water heater because emphysema patients tend to lose the capability to judge temperature. Secondly, inbvest in remote care technologty ti enable the nurse get alerted anytime the patient makes movement. Third, install motion-sensor lights and night lights in the patient’s room. Proper PPE precautions would include using disposing blood-stained linen and using emesis bag where appropriate.
Review the vital signs on the ADDS/ MEWS chart. Discuss how these parameters relate to evaluating the severity of blood loss?
The MEWS score wold be used by the nurse to quickly determine the ddegree of disease of the patient, by looking at six parameters namely AVPU response, heart rate, blood pressure, temperature, SaO2, and other observations. A score of five and above would be stastically associated with increased prospect for death or admission to an ICU. An increasing score would generate an escalated response that would vary with increasing the frequency of the patient’s observations. A nurse would observe and review anyu change in OBS/MEWS score, and compare the variations between one OBS reading from another. For instance, the decline in blood pressure (BP), sudden loss of blood/body fluids from haematemasis which can result to hypovolemic chock-brief definition (Howarth, Warne & Haigh, 2014). The nurse would note that heart rate increases the moment the blood pressure declines because the heart vessels are vasodilated.
Review the medication chart and discuss the action of the drug prescribed for nausea.
The drug prescribed for nausea is to allow yhe nurse read and note down the criticalness of the patient’s illness. By using the OBS parameters, the nurse will use them to undertake a CXR with the patient. The reading on the medication chart would indicate the respiratory level of the patient in case the patient nurse wants to study the respiratory levels of the patient (Levett-Jones, 2013).
The RN asks you to complete a 12-lead ECG on Mr Barber. Please label PQRST on to the ECG strip below.
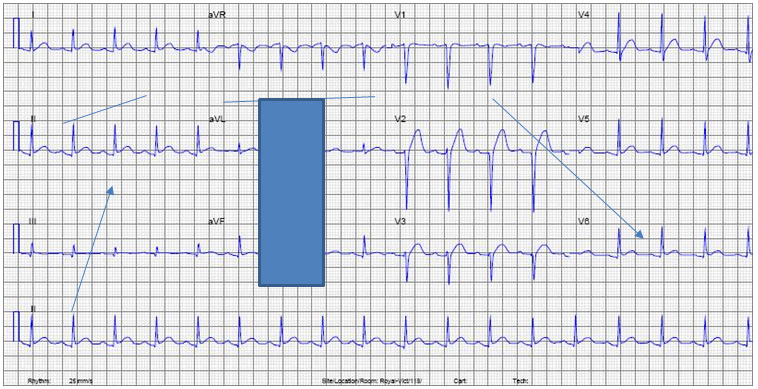
Use the information in the presenting history and patient charts to write your initial nursing report in SBAR format for Mr Barber. This report will be written 20 minutes after arrival when you have completed your initial assessment.
|
|
MRN: 0598371 Family Name: Barber Given Name: Frederick Date of Birth: 2/3/1931 |
PROGRESS NOTES |
||
|
Date/Time
|
S |
This is the patient’s situation: Mr. Barber has been having increasing emphysema, and has been complaining of continuous chest pains and coughing. Mr. Barber’s suffers from breath difficulties and his oxygen saturation has fallen to 85% on room air. |
||
|
B |
The background information is that Mr. Barber had a total knee replacement one month ago. Upon arrival at the hospital, Mr. Barber started complaining of chest pains. His pulse was 125, and his blood pressure was 120 over 68. Is noticed that he was restless and short of breath. |
|||
|
A |
To the best of my assessment, this patient might be having a pulmonary embolism or a cardiac event. |
|||
|
R |
I thus recommend that the entire medic attend to him with all care, and if possible, to start him on a 02 stat. |
|||
Mr Barber is upset that his wife is unable to accompany him to the hospital because she isn’t well. Give three questions you could use in your conversation with Mr Barber that would evaluate her safety to remain at home whilst he is in hospital. Ensure that your questions are phrased to take into consideration empathy, cultural or spiritual elements.
Is there any need, Mr. Barber, for your insistence to have your come here if you well know that the is unwell at home, and her coming here with you might worsen the situation considering the fact both of you need medical help and personal centered care?
Do you think it is necessary to have to allow your go home to be taken care of by your wife, or remain here for professional help, if indeed your wife’s warmth and love is what you feel will alleviate the pain?
c. How supportive is your family, especially your wife, emotionally, spiritually and mentally?
The neighbour looking after Mrs Barber telephones the Emergency Department and asks how Mr Barber is going. How would you respond to this telephone call as the nurse caring for Mr Barber?
Hello, you are calling the Emergency Department. Mr. Barber is recuperating eventually, but he needs more time before being discharged. The doctor has ordered an X-ray to be done on him by the course of today. By 20.40, Mr. Barber is supposed to be taken to the radiology department for further examination. Once all these two processes have been done on him, we shall establish the wayn forward. I assure you that we would protect the privacy and confidentiality of our patient.
Outline the preparation required to transfer Mr Barber to the radiology department for these tests. Include the following aspects in your answer:
What type of consent is required for this procedure?
The first consent we need should come from Mr. Barber himself, and ask him is he is willing and free to undergo the entire process of radiology testing. Before Mr. Barber is transferred to the radiology department, he is the first one to consent to the procedure. He must be told all the stages involved during the entire process. Next, the doctor should recommend him to be taken to the radiology. The doctor must specify the tests to be conducted to the patient.
Review the categories on the ADDS/ MEWS chart and identify the number and qualifications of staff members that should accompany him to radiology. Base this answer on your evaluation of his level of acuity and manual handling requirements.
We will base this on the OBS parameters and determine the suitable staff to go CXR with the patient. We would require a RN nurse to escort the patient and a motorized bed pusher since the patient would be pushed to the radiology room. Those accompanying the patient should be able the patient who is light headed and not able to stand or use the wheel chair. The staff members that should accompany Mr. Barber should be equipped with the knowledge of radiology. From the indication on the ADDS/MEWS chart, it is clear that the patient is delicate and only certain staff can understand and handle him. The fact that Mr. Barber’s movement is unsteady coupled with throwing the legs, he should be driven with care. Since he easily pushes the buzzer, it is evident that he is vomiting blood and this requires care with those who will organize the tools and equipment to use for radiology. IT technicians should also be involved in the process, whereby they will employ their IT knowledge during the radiology tests.
What is your response to this emergency?
I will apply the DRSABCD (Dimond, 2002).
D-Danger: I will check any danger around the person. I would be careful not to risk thje life of the patient while assisting him.
R-Response: I will check the consciousness of the patient, if he responds when I talk to him, and do some activities on him such as squeezing his shoulders and touching his hands.
S-Send for help: I will request for the help of the necessary assistance from the medical personnel around the hospital.
A-Airway: I will ensure that the patient’s airway is clear and that the person is breathing normally.
B-Breathing: By observing the patient’s chest movements, I will ensure that the patient is breathing properly.
CPR-Cardiopulmonary resuscitation: Just in case the patient would not be breathing normally, I will ensure that they lie flat on their back and then I will place one hand on the center of his chest and the other on top. I will then press smoothly and firmly 30 times.
D-Defibrillator: Just in case the patient turns out to be unconscious, I will apply an external defibrillator (this machine sends out an electric shock and cancels any chances of irregular heartbeat). (Dimond, 2002).
Explain to Mr Barber in simple terms how the actions of this drug relate to the pathophysiology of emphysema.
First, the patient should be given Seretide which works effectively within the lungs since the patient is suspected of having emphysema. Seretide works by releasing strong forces that combat the spread of of emphysema. The results from the examaination done on Mr. Barber would reveal a lot of issues. Emphysema would be diogised by lung-function and x-ray tests as seen in this case. Seretide adminsteresed during the chest X-ray of Mr. Barber is bound to show typical changes of emphysema. Suc include would include formation of holes (bullae), scarring, and enalargement of lungs. These changes would not appear until pulmonary functioning tesating has been carried out. The treatment conducted using drug dosages given to the patient after coming from the microbiology deparment would treat breathing complications and relieve any symptoms in the patient.
List the steps to correctly administer this medication.
Oxygen therapy done to treat emphysema symptoms. This therapy introduces the nurse practitioner to understand the patient in a more detailed manner.
Respiratory therapy done to treat any symptoms of emphysema;
Doing surgery to the patient (if appropriate);
Emphyema prognosis; and finally
Emphysema prevention to prevent occurrence at later stages.
Please read Mr Barber’s medication chart. Identify which of these medications would be used to treat the pain from his osteoarthritis (OA) – briefly describe the actions of this drug.
The medications for OA are given to reduce the level of pain, swelling, and stiffness. Medications for OA can be given to the patient in form of pills or syrups. The first one includes analgesics which are in form of pain relievers and should be given and taken by the patient through the doctor’s prescription. The second class of medication is non-stereoidal anti-inflammatory frugs that are meant to ease related pain and inflammation, and mostly include celecoxib, ibuprofen, and asprin. The third category is hyaluronic acid which acts as a lubricant and as a shock absorber. Another good class of medication includes corticosteroids which act as potent anti-inflammatory drugs (Cacchione, Eible, Gill & Huege, 2016). The patient will be given to take them by mouth or could even be inhected directly into the patient’s joint.
What questions might you ask him to help determine the severity of his OA and how the symptoms impact on his activities of daily living?
For how long have you been vomiting since the condition started?
So far, what changes do you have occurred in your body since you were introduced to osteoarthritis medication?
Do you feel that the medication we introduced you to, eased the pain you used to feel initially?
Now that vomiting has ceased, can you please explain any other thing you might be feeling in your body?
If we release you to go home, what do yu think your wife and family presence might do to relieve your former state of pain?
Is your reason for declining undergoing gastroscopy related with your wife’s ailing condition at home? Do you feel like being released to go home is the best idea for you?
Is there something you do not understand by now, and may require further explanations from the doctor?
What actions should you take now that Mr Barber has decided not to proceed with his gastroscopy?
I will apply the skill of compassion, which in this case I determined to use it to handle a patient who has entered an unfamiliar territory. I would further encourage my fellow staff members to consider and ensure that this patient’s dignity and respect are upheld. For instance, covering up the patient very well and all the time asking for his consent in case one of us wanted to enter their bed space. I will try hard to reason with Mr. Barber to see reasons for him undergoing another alternative gastroscopy now that he has refused undergoing the scheduled test. I will invite the RN and the leading doctor to come and discuss with the patient regarding the moral aspect to take.
What community assistance would be available for Mrs Barber whilst Mr Barber remains in hospital? Give an example of an allied health care worker who would make these arrangements prior to Mr Barbers discharge.
From the look of things, Mr. Barber can only agree to admission to the hospital once the arrangements for his wife have been provided. While Mr. Barber is being cared for, all the procedures and policies that were in place at the hospital were strictly followed. The patient should be given all the necessary treatment with a high standard of care and all the necessary alternatives to enable him communicate freely. The ethical issues of our patient’s understanding of what was happening at that time would be taken into consideration by all sources of communication to enable him be in control of his body and to consent to every phase of medical care (Bayne, Neukrug, Hays & Britton, 2013).
References
Bayne, H., Neukrug, E., Hays, D., & Britton, B. (January 01, 2013). A comprehensive model for optimizing empathy in person-centered care. Patient Education and Counseling, 93, 2, 209- 15.
Cacchione, P. Z., Eible, L., Gill, L. R. L., & Huege, S. F. (January 01, 2016). Person- Centered Care. Journal of Gerontological Nursing, 42, 5, 11-18.
Dimond, B. (2002). Legal aspects of patient confidentiality. London: Allen Publishing.
Howarth, M., Warne, T., & Haigh, C. (January 01, 2014). Pain from the inside: understanding the theoretical underpinning of person-centered care delivered by pain teams. Pain Management Nursing : Official Journal of the American Society of Pain Management Nurses, 15, 1, 340-8.
Levett-Jones, T. (2013). Clinical reasoning: Learning to think like a nurse. Frenchs Forest, N.S.W: Pearson Australia.



